Search
closeSimplifying the claims process on UHCdental.com
Q3 Word of Mouth newsletter 2022
New functionality on UHCdental.com helps simplify administrative tasks. The insight you’ll gain into a patient’s eligibility makes it easier to submit complete and accurate claims when documentation is required.
Enhancements to the provider portal include:
- The Eligibility Summary page displays information regarding missing tooth clauses
- The Benefit Details section includes a Waiting Period Met Date column
- The Claims Submission page shows clinical alerts and status display if a CDT® code requires additional information
Missing tooth clause
After logging in to UHCdental.com, you’ll see a statement on the member’s Eligibility Summary page that UnitedHealthcare Dental plans do not include a missing tooth clause. Patients covered by a plan with a missing tooth clause means the plan will not cover the costs of replacing the tooth if the tooth fell out or was extracted before the current dental coverage started. This is universal to all UnitedHealthcare Dental plans and will appear on every members’ Eligibility Summary page.
Waiting Period Met Date column
A new column showing “Waiting Period Met Date” has been added to the “Coverage and Deductible” tab on the Eligibility Summary page. A date will display showing when the member’s waiting period was met, or the field will show “N/A” if the waiting period has not been met.
Clinical alerts and status display
The Claims Submission page displays 2 alerts if additional information is required for specific CDT codes. These appear when you:
- Enter a procedure code that requires additional review
- Submit a claim without uploading the required documentation
An alert will display when entering a code for a claim or pre-treatment estimate if the code requires DDS review. The Exception Code box will display the code and a note in the footer will indicate “*Procedure requires DDS review.”
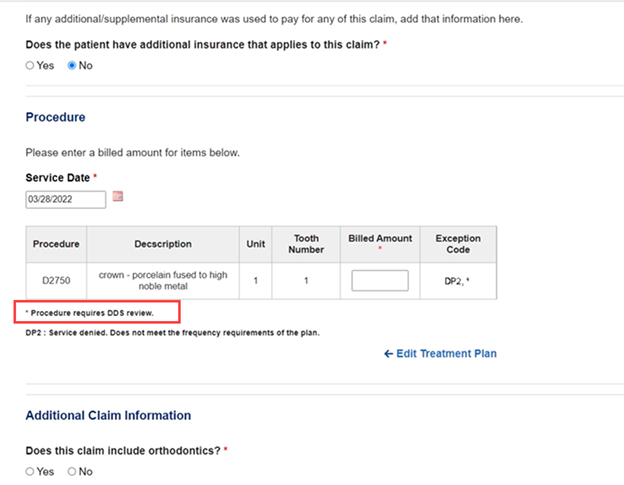
If you submit a claim without including the attachment, a pop-up will alert you that documentation is required.
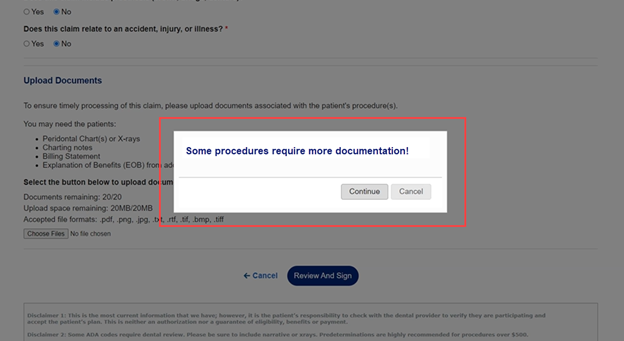
After the Claim/PTE has been submitted, the status section of the Claim Details page will indicate when a clinical review is pending.